
Value-Based Care: Payer Relations
Value-Based Care: Payer Relations
Data sharing is enhanced between providers and payers in a value-based contracting (VBC) relationship through the design and implementation of a data and technology strategy. Is your organization ready?
VBC models require deep collaboration between healthcare providers and their payers. There must be shared objectives, measures and outcomes. Data, information and results must flow freely. In addition, risk must be allocated appropriately. In this environment, success very much depends on the strength of your payer relationships.
In today’s fee-for-service world, most providers treat all their payers as equal. Few truly understand which payer relationships are performing the best. Fewer still are engaged in a constructive two-way dialogue with their payers about their performance.
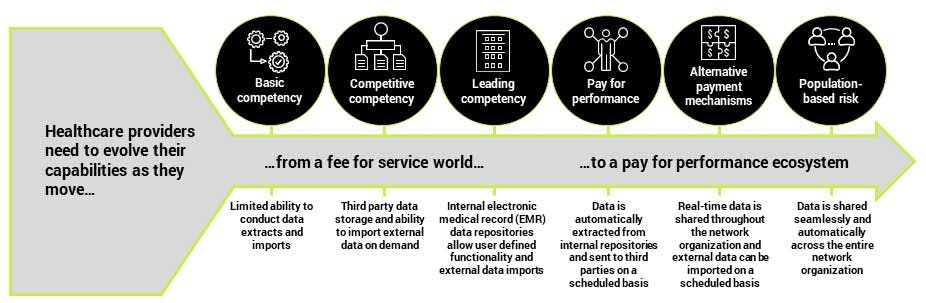
Understanding and shaping payer performance is key to developing the types of collaborative relationships necessary for success as providers take on more risk. Particularly in the early days of VBC contracting, providers will want to be very selective about which payers they work with. Furthermore, they will want to start enhancing those relationships as soon as possible.
Five key considerations
1. Manage your payer performance: Develop a robust payer performance management program empowered with the right tools, capabilities and processes to properly assess the comparative value of your various payers. Go beyond traditional volume and revenue measures. Continuously assess key metrics on an ongoing basis. Engage payers in constructive dialogue about performance improvements.
2. Take it to the C-suite: The leading providers view payer performance and payer relationships as a C-suite agenda item. Engage your executives – and your payers’ executives – in the shift towards the development of VBC models. Ensure progress towards VBC contracting aligns with the organization’s overall strategy.
3. Expand your contact list: Don’t rely on your current payer contacts to “grow with you” as you evolve. Proactively identify the various stakeholders responsible for VBC model development – including contacts in IT, operations and strategy.
Work with them to cultivate relationships and build the strategy towards greater use of VBC models.
4. Build your data capabilities: Reassess your current data models and capabilities to prioritize data integration and analysis, both internally and externally. Ensure you have robust controls over your data, its access and its management. Given that most payers’ systems and data protocols are different, focus on building “open data” technology architecture.
5. Develop new capabilities: Consider what capabilities will be required in order to manage the full life cycle of a payer relationship. Develop, recruit or retain key VBC contracting and negotiation capabilities, as well as predictive analytics and actuary skills. Work with IT to enhance data and analytics capabilities.
“Even absent a wholesale shift to VBC, market trends suggest that the relationship between providers and payers is becoming much more dynamic. Improved data sharing, collaboration and performance measurement will deliver value today and in the future.”Michael Patti, Principal, Baker Tilly
Two minute self-assessment
Ask yourself whether …
- You have a comparative view of how each of your payers are currently performing? Are your resources focused on the right payers?
- Your current contracts with commercial health plans include indicators for clinical quality, patient experience or efficiency performance?
- You have the right relationships with the people at your key payer organizations responsible for driving value-based care contracts?
- Your organization has the right skills and capabilities to create, negotiate and manage value-based contracts with payers?
- You have a robust care management organization (CMO) with a mandate to drive payer negotiations for value-based care contracts?
- You have access to the payer data you need to properly assess, predict and manage your risk-based contracts?
If you answered “no” to any of these questions – or if you just don’t know the answer – you may not be ready to assume the risk required to successfully move towards value-based care. Talk to us to find out how you can become ready.
How Baker Tilly can help
Baker Tilly’s team of Value Architects™ provide management consulting, technology and financial planning for healthcare organizations across the health plan, provider and life sciences spectrum.
Our healthcare professionals understand how to drive collaborative value-driven relationships with payer organizations. From helping providers develop and improve their payer performance management process through to designing and implementing the data and technology strategy to support enhanced data sharing between providers and payers, our team of professionals have a proven track record for helping provider organizations create the type of payer relationships they need to thrive in a VBC environment.
Contact us today to find out how Baker Tilly can help your organization.














