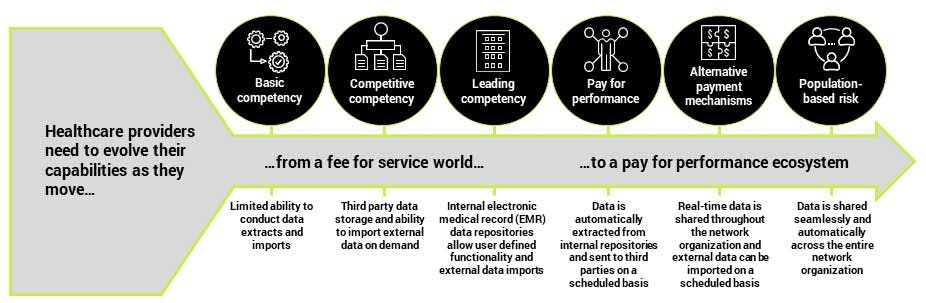
In a utopian VBC world, information and data would flow freely between payers, providers, third-party network organizations and patients. Decisions would be based on complete patient information in real time. External data sources such as social determinants of health and population health measures would be continuously integrated into the data stream. Payers and providers would have clear and continuous insight into how they are performing across a wide range of measures.
Today, however, most providers are struggling to share information within their own facilities, let alone with their payers or third-party network providers. Gathering payer data from multiple portals, integrating it with internal and external data sources, and then sharing it across the network organization is an immense challenge.
The shift to VBC may offer providers an opportunity to rethink the way they collect, share and manage data today and in the future.